Functional Diaphragms: The Overlooked Transition Zones That Posture Can Quietly Disrupt
When most people hear the word diaphragm, they think of breathing. They think of the large dome-shaped muscle under the ribs that helps move air in and out of the lungs. Although that is true and important, the root meaning of the word tells us more.
The word diaphragm originally points to the idea of a partition, a dividing structure, a region that separates spaces while also regulating what passes through them. This is often veins, arteries, nerves, or lymph vessels. Which goes far beyond just breathing.
The body has multiple regions that act like functional diaphragms. These are transition zones. They are bottleneck areas. They are places where pressure, tension, fluid movement, circulation, lymphatic drainage, nerve mobility, and posture all have to work together.
If those spaces stay open, adaptable, and calm, the body tends to move fluid better and feel better. If those spaces become compressed, guarded, or chronically overloaded, the body starts to lose efficiency. That is often when discomfort begins to show up, even if the real problem has been building quietly in the background for a long time.
This is one of the reasons we pay so much attention to what we call functional diaphragms.
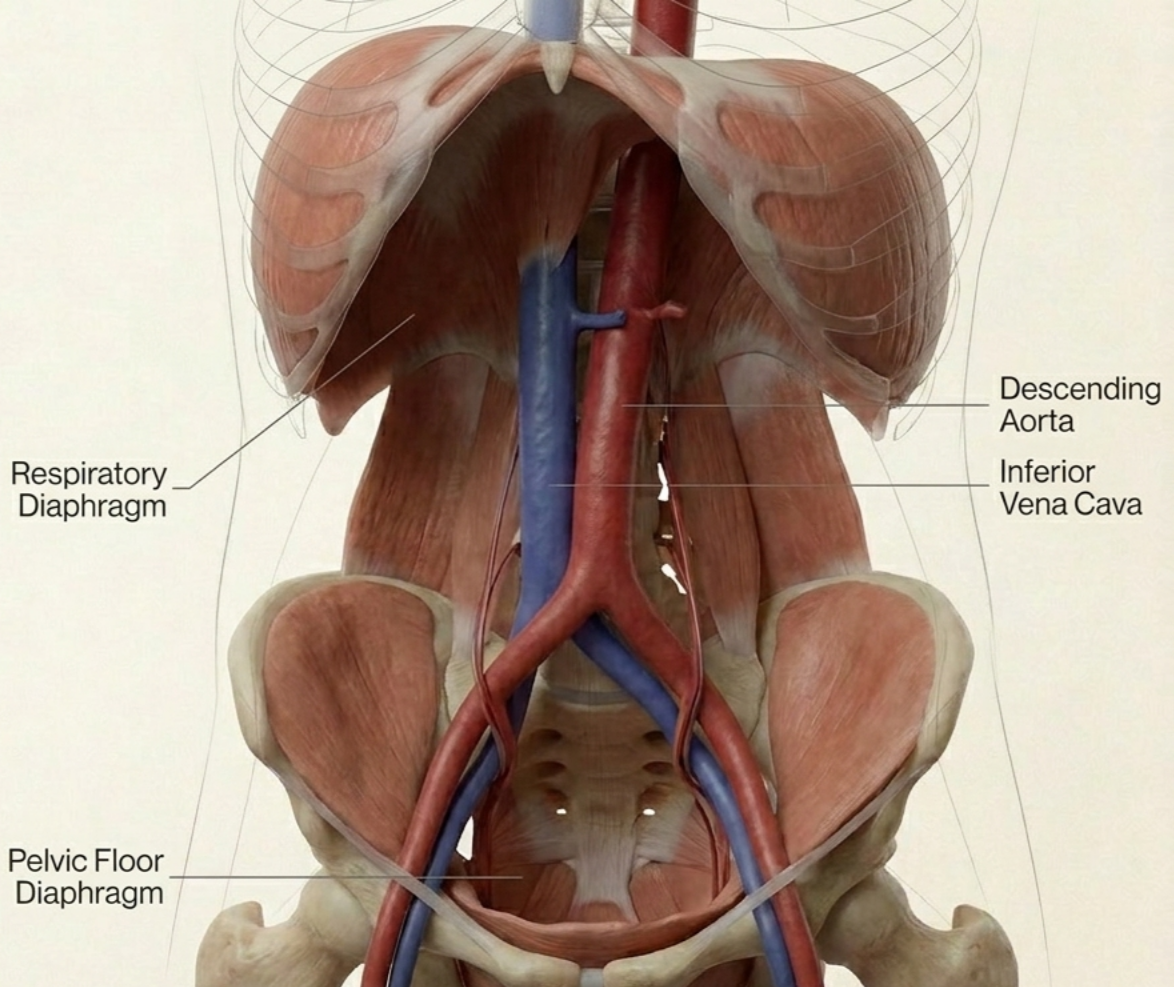
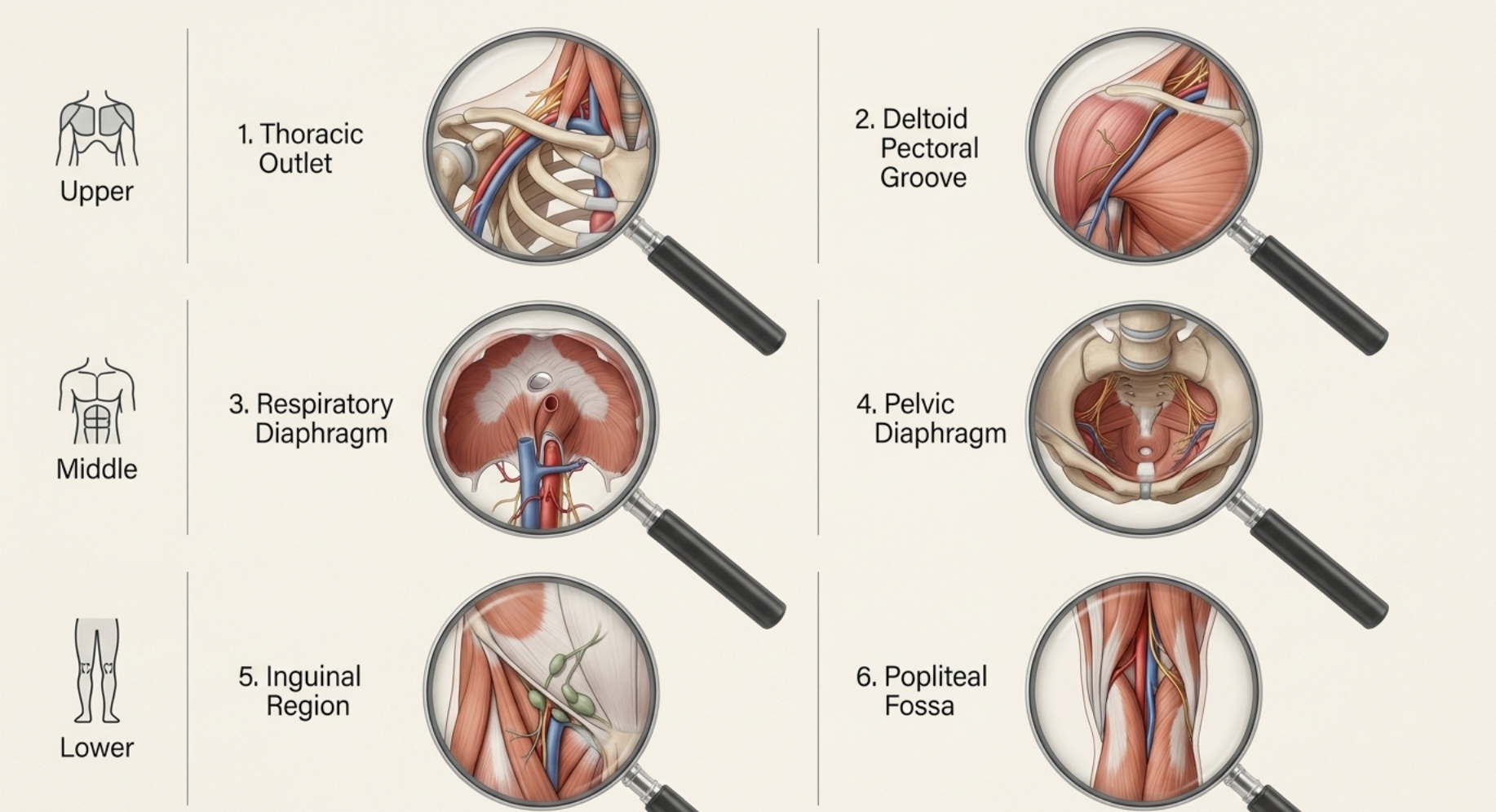
The ones we think about often are the thoracic outlet, the respiratory diaphragm, the pelvic diaphragm, the femoral triangle, and the popliteal fossa. Each one serves as a key passage point. Each one can be influenced by lifestyle, training, stress, work posture, and even sleeping position. Each one can become a place where the body starts to slow down, stiffen up, and protect itself.
That protection matters, because protection often comes before pain.
We say that a lot because it keeps proving itself true. Protection precedes pain. The body almost always tries to defend itself before it starts screaming for attention. Hypertonicity is protection. Inhibition is protection. Tenderness is often protection. Reduced motion is protection. The body is doing the best it can with what it has.
The problem is that if protective tone stays too long, it starts to create a new environment inside the body.
A region that should feel open and adaptable starts to feel dense. Muscles that should coordinate well begin to feel overactive at rest and underperforming when asked to work. Fascia becomes less forgiving. Blood flow can slow down. Venous return can become less efficient. Lymphatic movement can become sluggish. Local irritation can increase. Tenderness rises. Stagnation begins to build. Then that stagnation feeds even more guarding.
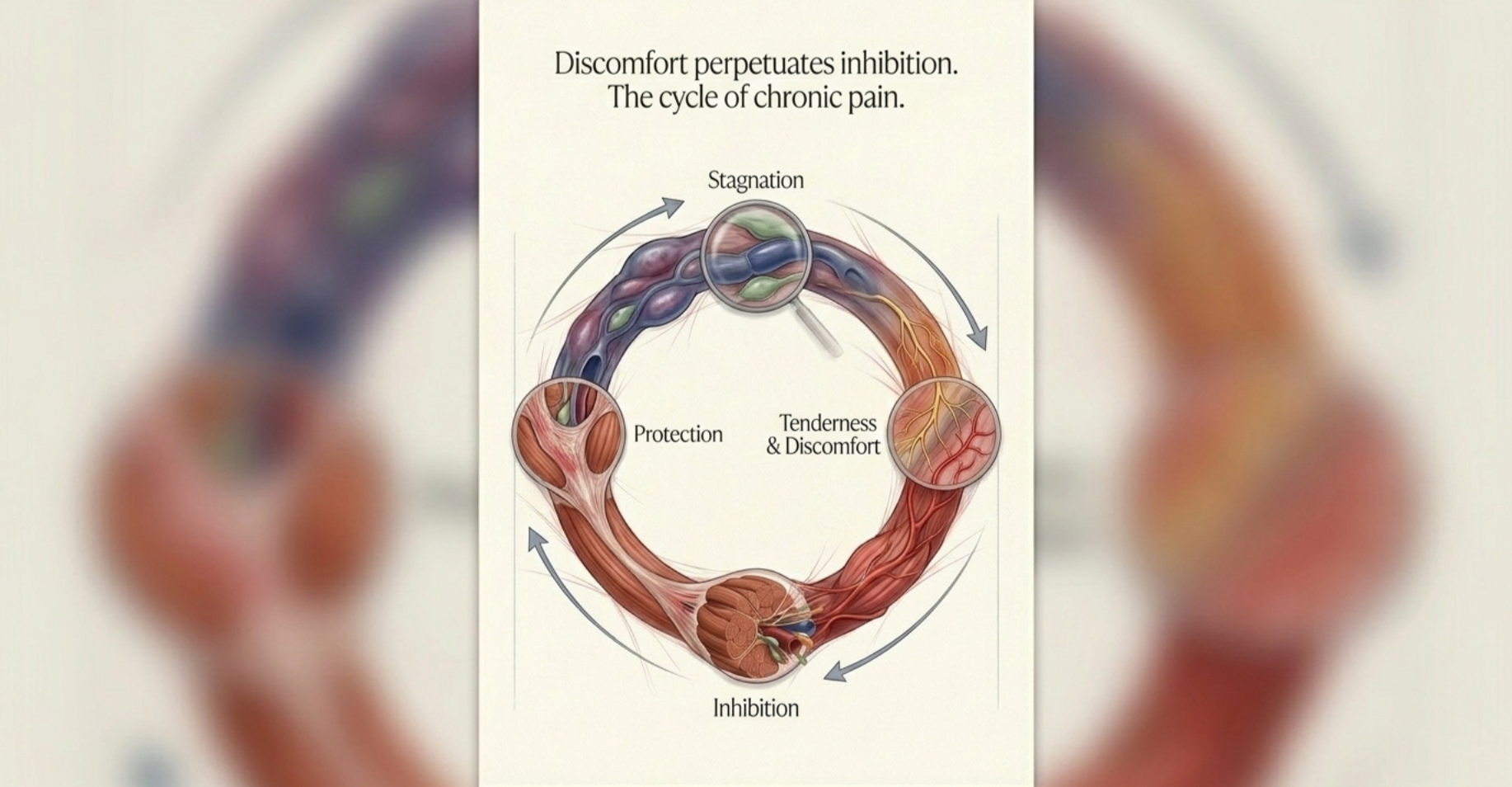
That is the loop.
Tenderness can signal hypertonicity. Hypertonicity can slow blood flow and lymph flow. Slower flow can increase stagnation. Stagnation can increase discomfort and tenderness. That tenderness can reinforce even more protective tone and altered movement. Over time, the body starts living inside a cycle that feels normal until it becomes painful enough to interrupt life.
This is why posture matters more than people think.
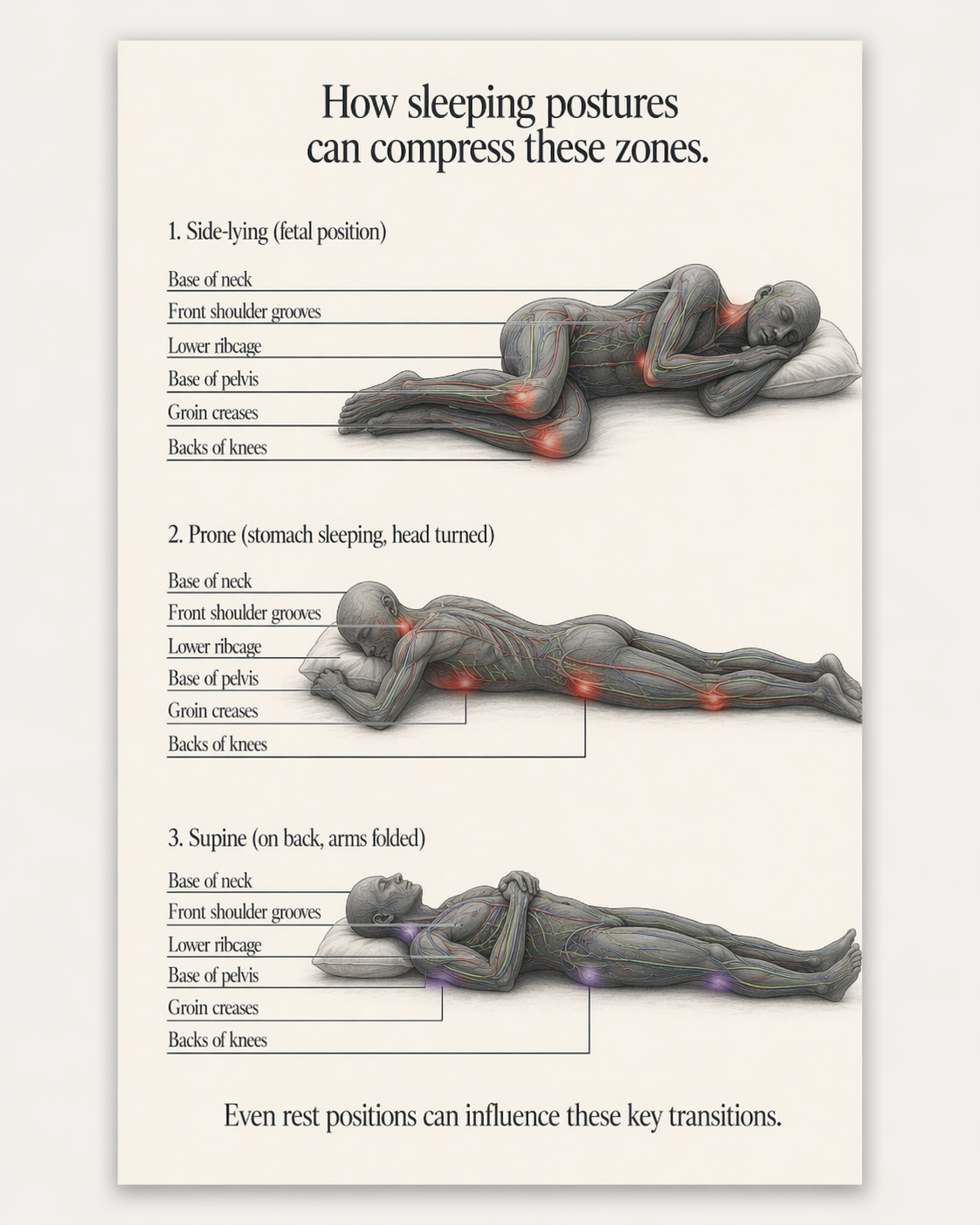
When we say posture, we do not just mean standing tall or sitting up straight. We mean repeated positions. We mean how long your shoulders stay rounded while working at a desk. We mean how many hours your hips stay flexed while driving. We mean whether you always sleep with one arm overhead, whether you collapse into one side, whether your ribcage stays compressed, whether your neck never really gets a break, whether your groin is always under tension, whether the backs of your knees never fully move through healthy ranges.
Lifestyle posture is not just about appearance. It is about pressure over time.
One of the clearest examples of this shows up around the thoracic outlet. This area is often discussed in the context of thoracic outlet syndrome, which is multifactorial and can involve ribs, clavicle mechanics, scapular position, the scalenes, vascular structures, and neural structures. That is true. It is a complex region. But even before a formal diagnosis enters the picture, this area can still become a functional bottleneck.
If the tissues around the lower neck and upper chest stay tense for too long, the body can begin to narrow the space where important structures need to pass. Sometimes the issue is not dramatic enough to be labeled in a classic diagnostic way, but it is enough to make someone feel heaviness, tension, superficial discomfort, tenderness, altered sensation, or a vague sense that the area just never feels open.
The same principle can show up lower in the body.
The femoral triangle is another region where multiple structures need room to move and glide. If the abdomen, obliques, hip flexors, adductors, or surrounding fascial tissues stay hypertonic, the groin can become another place where the body starts losing fluid efficiency and mechanical freedom. The popliteal fossa behind the knee can become a similar story. If the tissues above and below it are stiff, irritated, or overloaded, that transition point can become less adaptive.
These zones are not random. They are intersections. They are checkpoints. They are places where the body either keeps things moving or starts slowing things down.
That brings us back to fascia.
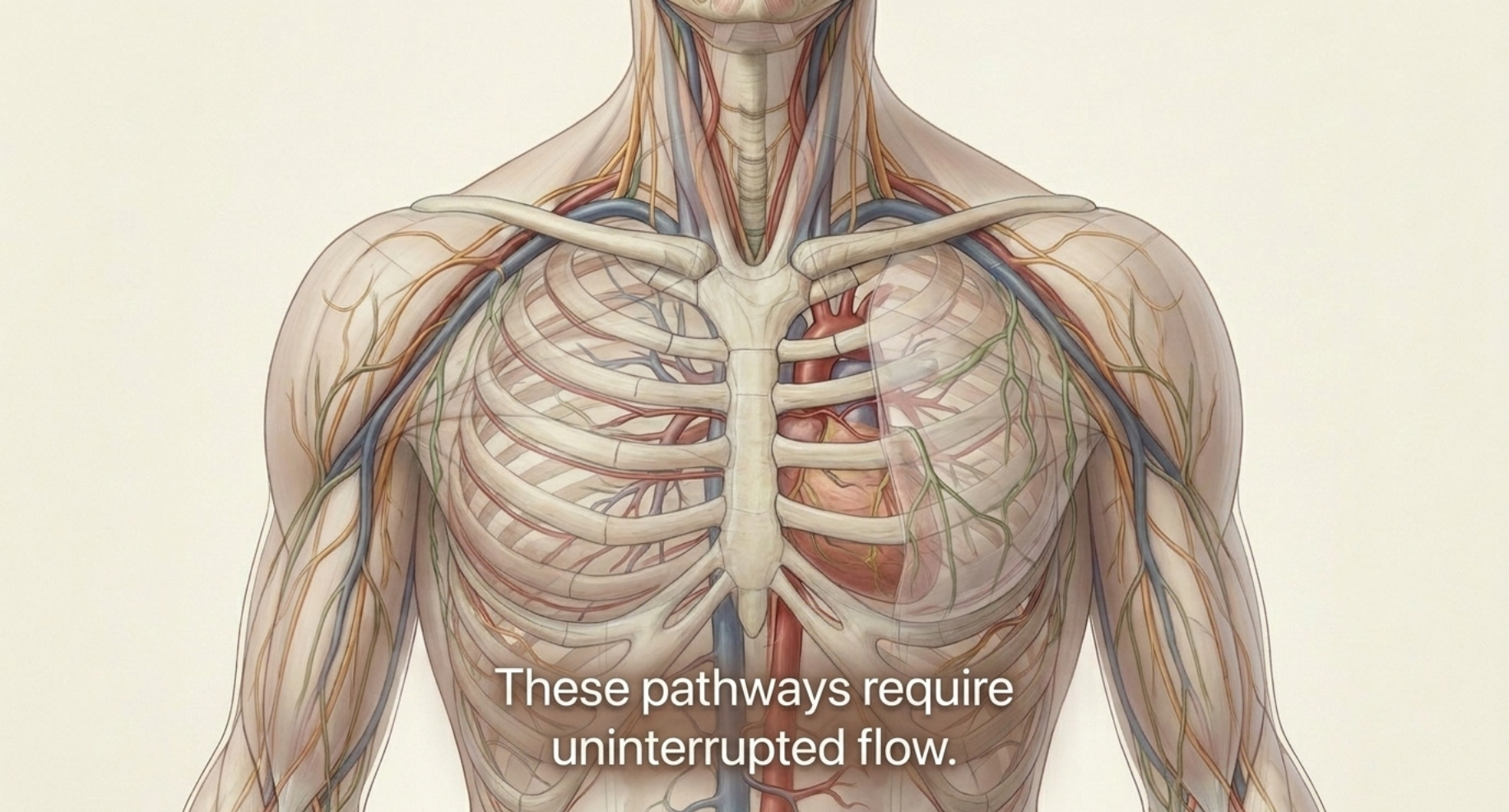
A lot of the time, fascia gets discussed only in relation to muscle tightness or mobility work, but fascia also matters because it helps organize space. It helps create pathways. It helps support how bundles of vessels and nerves travel through the body. Major arteries, veins, and nerves often travel together in organized regions supported by deeper fascial layers. If that fascial environment becomes restricted, thickened, dehydrated, overloaded, or compressed by hypertonic muscles around it, the body can start to lose some of the fluid ease it needs.
That does not mean every tender spot is a trapped vessel or a major pathology. It means the environment matters.
The body needs more than strength. It needs space. It needs glide. It needs pressure management. It needs regulated tone. It needs healthy movement of blood, lymph, and nerves through regions that are designed to be transitional.
And blood flow itself deserves more attention than it usually gets.
We are used to checking blood pressure. We talk about how well the heart pumps blood out. But people do not spend nearly enough time thinking about how well the body helps move blood back. Venous return is a huge part of feeling healthy. Lymphatic return is a huge part of recovery. The body relies on movement, muscle tone, pressure changes, breathing mechanics, vessel integrity, and autonomic state to support these systems.
If muscles are too hypertonic, they can become less helpful. Instead of assisting the movement of fluid, they can become part of the resistance. If someone lives in a more chronically stressed state, the body can stay less parasympathetic and less efficient with drainage and recovery. If breathing is shallow and the ribcage never really expands well, that affects pressure systems too. If someone hardly moves all day and then sleeps in a compressed posture all night, they may be stacking stagnation on top of stagnation.
Then they wake up wondering why they feel stiff, swollen, heavy, achy, or irritated for no obvious reason.
This is where hands on work can become valuable.
Sometimes what a body needs most is not more force but better input. Warm hands, specific pressure, and careful attention to a tender zone can help the nervous system soften its grip. Not by attacking the body, but by communicating with it. Not by trying to overpower protection, but by understanding it.
That is an important distinction.
We do not look at tenderness and think, this needs to be crushed out. We look at tenderness and think, this region is telling me something. This area may be asking for space, for calm, for better drainage, for better pressure management, for improved awareness, for improved breathing, for reduced guarding.
Sometimes that means direct manual therapy. Sometimes it means restoring diaphragmatic breathing. Sometimes it means changing work posture. Sometimes it means sleeping differently. Sometimes it means getting out of one repetitive pattern more often during the day. Sometimes it means improving hydration. Sometimes it means recognizing that a body living under chronic stress is also living under chronic tone.
When the body becomes less congested, it often becomes less defensive.
That is why working these functional diaphragms matters to me. We’re not just thinking about where pain is. We’re thinking about where things may be getting stuck. We’re thinking about where the body may have lost some of its ability to circulate, drain, rotate, expand, descend, return, and recover.
A healthy body is not just a strong body. It is a body that can move things well.
It can move air well. It can move blood well. It can move lymph well. It can move nerve structures through space well. It can change pressure well. It can transition from one posture to another well. It can adapt well.
When those transitions are lost, symptoms begin to accumulate. When those transitions are restored, relief often follows.
That is why we think these functional diaphragms deserve more attention.
The thoracic outlet deserves attention.
The respiratory diaphragm deserves attention.
The pelvic diaphragm deserves attention.
The femoral triangle deserves attention.
The popliteal fossa deserves attention.
If there is one big takeaway here, it is this.
Pain is rarely the beginning of the story.
A lot happens before pain. Protection happens first. Changes in tone happen first. Changes in circulation happen first. Changes in posture happen first. Changes in breathing happen first. Changes in drainage happen first. Changes in adaptability happen first.
By the time pain shows up, the body has often been working very hard for a very long time.
So sometimes the best thing we can do is stop asking only, where does it hurt, and start asking, where is the body losing space, flow, and adaptability?
That question often leads us somewhere deeper.
And many times, it leads us right back to these functional diaphragms.